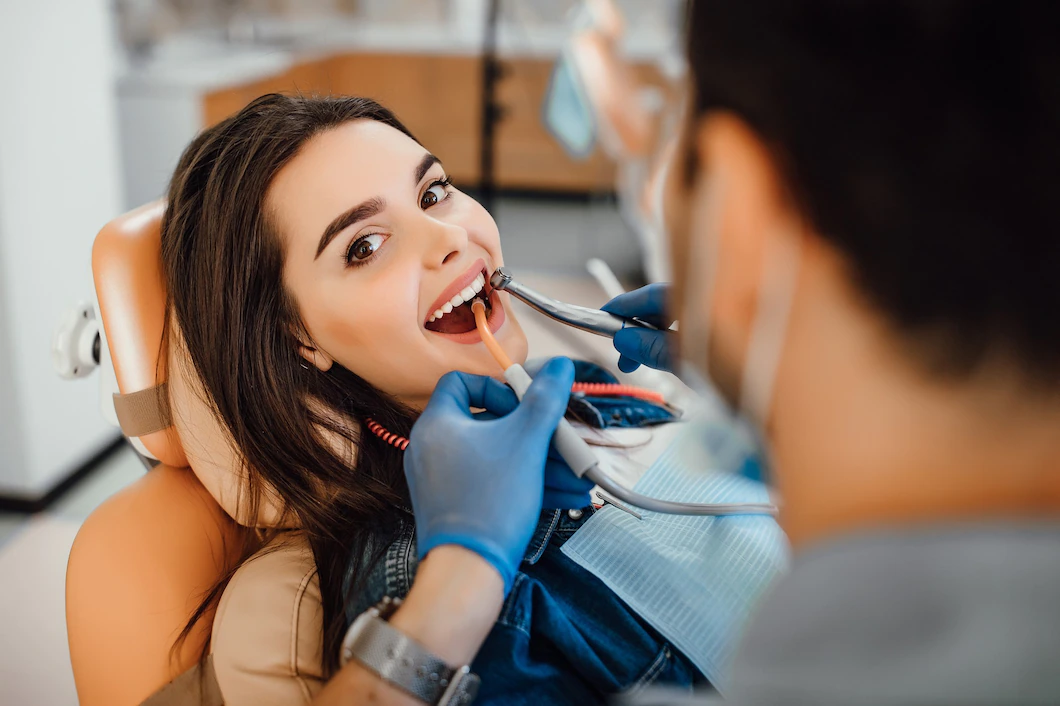
Periodontitis is a form of gum disease that is caused by plaque buildup and inflammation around the teeth and gums. It is chronic in nature, meaning it can last indefinitely without proper treatment.
It causes pockets of infection to form around the teeth and gums, which can lead to irreparable damage if left untreated. The infection destroys gum tissue, bone tissue, and ligaments that hold teeth in place – eventually leading to tooth loss.
Symptoms

Common symptoms of periodontitis include red, swollen, or tender gums; bleeding from brushing or flossing; receding gums; changes in how your teeth fit together when you bite; bad breath; and/or pus between your teeth and gums. In severe cases, loose teeth or pain when chewing may occur. If left untreated, periodontitis can cause your teeth to fall out or need to be removed altogether.
Causes
Periodontitis often starts with an issue that is caused by inadequate oral hygiene. Plaque and tartar will build up in areas between teeth and gums and create an environment that is favorable to bacteria growth. These bacteria can cause inflammation of the gums (a condition called gingivitis) which will lead to periodontal disease if not remedied.
Other causes of periodontitis include smoking, genetics, a weakened immune system, an insufficient diet, changes in hormones from conditions like pregnancy or menopause, ill-fitting dentures, foreign objects between the teeth such as trapped food particles, or a misaligned bite. Conditions like diabetes can also make it more likely for one to develop periodontitis due to complications caused by higher levels of sugar in the saliva.
Can Periodontitis Be Cured Permanently?
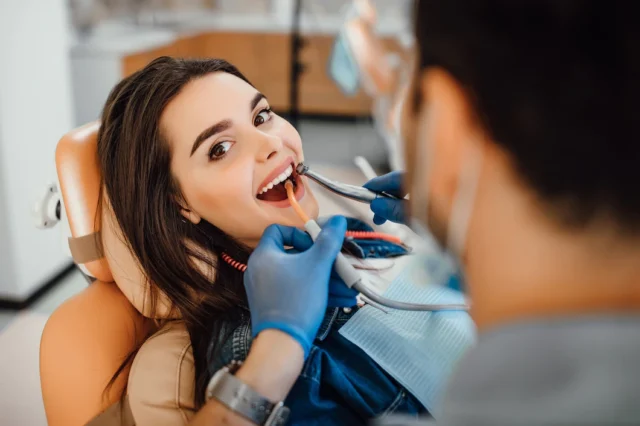
The good news is that periodontal disease can be cured with proper treatment from a periodontist. However, it’s important to note that curing periodontitis does not necessarily mean it’ll never return. Treatment will help slow down the progression of the disease and may even reverse some of the damage already done.
Non-Surgical Treatments
Non-surgical treatments have been suggested as a way to treat more serious cases. These treatments are intended to stop the progression of the periodontitis, but may not always lead to a permanent cure. Non-surgical treatments include:
1. Professional cleaning and dental scaling: This process involves the removal of plaque, tartar, and other bacteria from below the gum line that contributes to gum disease.
2. Antibiotics: Antibiotic medications can be used to control the growth of harmful bacteria in the mouth that contributes to periodontitis.
3. Medications: Special mouth rinses or gels are available that can help reduce inflammation and control the spread of infection caused by this disease.
4. Local anesthesia: Applying an anesthetic agent around teeth involved with periodontitis can help reduce sensitivity during certain treatments such as professional cleanings or scaling procedures.
5. Laser therapy: Laser therapy is one way to remove bacteria from deep areas around teeth, but it also can help increase blood flow, allowing for more effective healing.
Choosing non-surgical treatments is often beneficial when the infection has advanced beyond what can be treated by brushing alone and it becomes important for a patient’s oral health in general too; however, many cases require more intervention than just non-surgical fixes and may require surgery in order to permanently cure advanced or recurring cases of periodontitis
Surgical Treatments
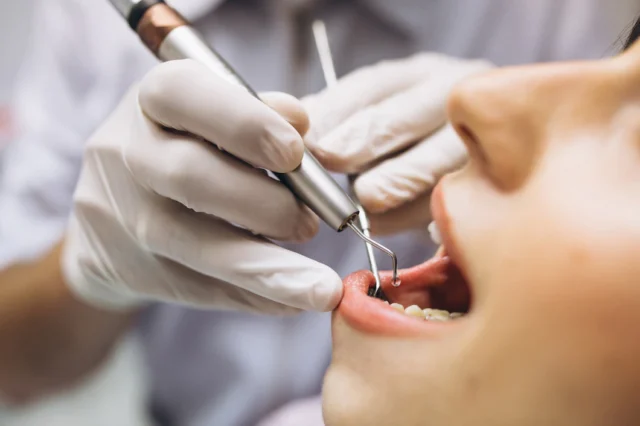
In addition to non-surgical treatments like antibiotics and scaling, periodontal diseases may require more extensive surgery if the pockets are deep, and have extensive damage from the disease, and other factors. Possible surgical treatments may include:
• Gingivectomy/Gingivoplasty: During these procedures, the infected tissue around your teeth is efficiently removed or reshaped to reduce pockets.
• Soft Tissue Grafts: When your mouth doesn’t have enough tissue due to severe gum recession, your dentist will replace it with healthy tissue taken from another part of your mouth or use a synthetic substitute such as a collagen membrane.
• Bone Grafts: This procedure replaces infected bone around teeth originating from a donor site in your jawbone or using a synthetic bone replacement material.
• Guided Tissue Regeneration / Guided Bone Regeneration (GTR/GBR): It’s used when pocket depth needs to be restored in advanced periodontitis cases. This technique is done by blocking some gum tissues and bone cells from getting into the space created during treatment so that regeneration has time to occur and new healthy tissues can grow back.
• Crown Lengthening / Soft Tissue Impression Coping (STIC) Procedure / Side Bos Posture: These surgeries are often necessary for cosmetic issues of replacing missing tissues not related to tooth decay, but usually needed by those undergoing dental implants when there isn’t enough bone structure exposed for implant placement.
Prevention and Management
Taking preventive measures such as practicing good oral hygiene and seeing your dentist regularly can help reduce your chances of developing periodontitis or lessen the severity of the condition if you already have it.
Good Oral Hygiene
Brushing and flossing are habits that should be incorporated into your daily routine in order to maintain a healthy mouth and prevent the buildup of plaque which can lead to periodontitis.
When brushing, it is important to use a soft-bristled brush and spend at least two minutes covering all surfaces of the teeth, including the backside. Additionally, make sure to brush at least twice a day—once in the morning and once in the evening—as well as after every meal or snack. Additionally, flossing should also be done daily or between meals. Be sure to use an 18” piece of waxed dental floss when flossing and don’t forget to clean between all teeth.
Using an antibacterial mouthwash can also aid in fighting off plaque-causing bacteria. If you’re tempted by sugary foods or drinks throughout the day, make sure to rinse your mouth immediately with water afterward as it will help dilute these sugars that attract bacteria.
Regular Dental Visits
Professional dental cleanings are your first line of defense against periodontal disease.
During these appointments, plaque and tartar buildup will be removed from the surface of your teeth. The tartar (hardened plaque) must be removed to ensure that the infection-causing bacteria underneath is taken care of as well.
Your dentist will also provide a thorough examination at each appointment in order to detect any signs of periodontal disease that may otherwise go unnoticed by you or your hygienist.
Regular visits help you keep up on your preventive care program, which can provide early detection of any changes in your gum health before they become more serious issues needing more intensive treatment options.
During regular visits, your dentist will also check for any indications of gingivitis (early stages of periodontal disease), an important precursor to progressing gum disease. Gingivitis can often be reversed with good home oral hygiene and professional cleaning by a dentist or hygienist, so catching it early helps prevent it from getting worse.
Diet and Lifestyle Changes

There are certain dietary and lifestyle modifications that can potentially reduce your risks for periodontitis or help control symptoms if you’ve already been diagnosed with gum disease. These include the following:
• Consuming a nutritious health-promoting diet that is low in sugar
• Cutting back on smoking or quitting altogether
• Adding stress management activities to your routine (yoga, meditation, deep breathing exercises)
• Increasing physical activity
• Utilizing nutritional supplements targeted for specific periodontal needs (omega 3 fatty acids to reduce inflammation, vitamin C for its antioxidant effects)
• Taking medications that help manage any underlying health conditions that may worsen periodontal disease (such as diabetes)
Conclusion
It is important to be aware that periodontitis can be a serious oral health problem and can often lead to damage to the underlying gum tissue. However, with consistent and appropriate dental care, it is possible for the initial symptoms of this condition to diminish and for further damage to the mouth and tooth structures to be prevented.