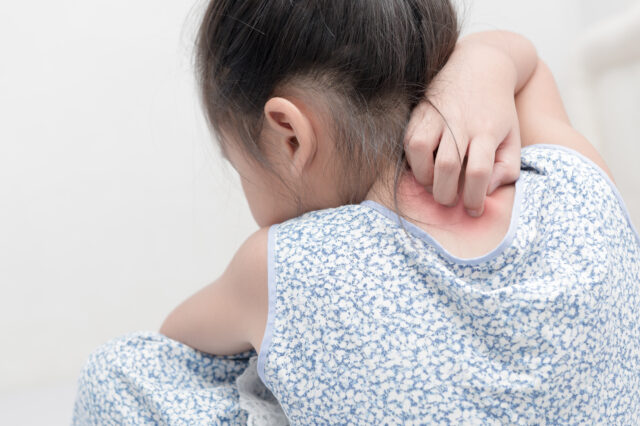
Atopic dermatitis in toddlers, and children in general, usually means eczema, although eczema is a broader group of skin conditions. People with this problem have very sensitive skin that is prone to infections.
As is the case with many other health conditions, it can be either acute or chronic. In the acute case, the skin peels off and fluid is secreted from the regions of the skin affected by it. In chronic, the skin looks dry, thickened (elevated) and dandruff occurs.
A characteristic symptom of this condition is itching. The very persistent, and annoying one.
However, it is important to know that this condition is not contagious. It cannot be transferred from one person to another, so rest assured other kids will be fine when interacting with your toddler.
It often occurs with two other allergic conditions: asthma and allergic rhinitis. Children whose parents or close family members have asthma or allergic rhinitis are more likely to develop it.
It is a relatively common skin disease that affects a wide population of people and is specific to urban and low-humidity environments.
The term “dermatitis” means that the condition involves inflammation of the skin, and the term “atopic” means that the condition is caused by an allergic reaction. People suffering from it have an unadjusted immune reaction, which is the case with allergies.
Like any atopic disease, it falls into the same classification as allergic rhinitis and asthma.
It usually begins in early childhood, most often in the first 6 months of a baby’s life. Most people develop it before the age of five.
It is the most common form of eczema and can be very severe and long-lasting. When your toddler suffers from it, in some periods it can completely withdraw, while in others it can get worse.
Many children with such conditions enter permanent remission when they grow up, although their skin still remains dry and prone to irritation.
There are several factors that encourage or worsen it, such as low humidity, seasonal allergies, exposure to soaps and detergents, and cold weather. Environmental factors can trigger the symptoms at any time in life in people who have inherited a predisposition to this condition.
Let’s take a closer look at all the factors that can trigger this condition in toddlers…
Even today, with all the breakthrough discoveries medicine has managed to come up with, the very reason this condition occurs in toddlers remains unknown. However, a couple of things that trigger it, remain a fact. We’ve listed them below…
It can be inherited. An interesting fact about it is that a toddler is more likely to inherit it from the mother, than from the father. A history of it in one parent has been shown to contribute to an increased risk of developing the same condition while in a toddler period of life.
Food allergies have not yet been ruled out as potential causes. The most problematic foods are milk, eggs, salt, peanuts, chocolate, gluten, and other cereal proteins and preservatives.
In addition to the food that triggers allergic reactions, an imbalance of the fat covering the upper layer of the skin can contribute to the development of this issue. There is also the possibility of the entry and development of pathogenic bacteria and fungi. There is a loss of fluid through the upper layer of the skin and later inflammation.
Then again, it can also be caused by a number of factors such as personal hygiene products, household detergents, contact with allergens, dust, pollen, hair, and feathers, chlorine from bath water, or hormones. So, in the end, you may conclude that almost anything your toddler has been exposed to can influence this condition, given the fact how broad what we wrote above is.
Since it’s so persistent, is there anything you can do about it?

Although after reading everything we wrote above, it may sound scary, some products can successfully help your toddler get rid of this condition, like the ones found on bioderma.com.au. But it can also be prevented by a simple change of habits. Below are some suggestions:
• Gentle washing and regular and effective hydration keep the skin soft and prolong the periods between the onset of symptoms.
• Use anti-inflammatory ointments and creams (after consulting a doctor).
• Avoid clothes and bedding made of wool and synthetics. Choose cotton or silk clothes and bedding for your toddler.
• Avoid washing clothes and bedding with “heavy” detergents, which contain perfumes, preservatives, and dyes. Choose liquid detergents and always wash clothes and bedding well.
• Rough detergents/baths can also damage the delicate protective layer and affect the toddler’s skin’s moisture balance.
• Avoid contact with the child with mites and dust as much as possible. Clean mattresses, bedding, carpets, and curtains regularly.
• Do not keep stuffed toys in the bed where the child sleeps and wash them regularly.
• Make sure that the air in the room where the child is staying is not dry and overheated.
• Do not smoke in the room where the child is staying.
• If you have a pet, wash it regularly and do not allow it to enter the room where the child sleeps.
• Regularly trim your child’s nails so that they do not damage the skin when scratching.
Paying attention to how you bathe your toddler is also important. Here’s what we suggest:
The first thing to pay attention to when your toddler is combating this condition is washing or bathing products you use. The water also must not be too hot (around 32-34 ° C) and bathing must be short (5-10 minutes). It is recommended to use products without soap that do not cause irritation. It is also important to rinse the skin well and gently dry it with adequate towels by tapping, avoiding rubbing. Also, avoid bubble baths.
As we’ve mentioned previously, although this issue can be very persistent and annoying, with a change of habits it can be controlled.